By Ticha
Group Therapy, Mental Health, Therapy
cbt for anxiety, cbt for depression, cbt interventions, cbt therapy, cbt therapy exercises, cbt therapy worksheets, cognitive behavioral therapy techniques, cognitive restructuring cbt, how cbt works
Overview of Cognitive Behavioral Therapy

Cognitive behavioral therapy (CBT) is a popular and proven-effective psychotherapy technique that helps people identify unhelpful thoughts and behaviors and learn skills to challenge or change them. CBT focuses on the present and aims to provide clients with tools they can use anytime to manage problems and feel better.
CBT is based on the idea that your thoughts, behaviors, and emotions interact and influence each other. For example, if you’re feeling depressed, you may have more negative thoughts and act in dysfunctional ways. These thoughts and actions can fuel your depressed mood. CBT helps break this cycle by teaching you to recognize and change thought patterns and behaviors.
This article provides a comprehensive overview of CBT. We’ll explain what CBT is, how it works, techniques used, effectiveness, types of CBT, and more. Let’s start with the basics.
What is Cognitive Behavioral Therapy?
.jpg)
Cognitive behavioral therapy (CBT) is a form of psychotherapy that focuses on modifying dysfunctional emotions, behaviors, and thoughts by interrogating and uprooting negative or irrational beliefs. CBT aims to solve problems related to dysfunctional emotions, behaviors and cognitions through a goal-oriented, systematic process.
The treatment focuses on how a person’s thoughts and perceptions affect their emotions and behaviors. CBT therapists work with patients to uncover, investigate and alter distorted thinking patterns and adopt positive mindsets that precipitate healthy actions.
CBT rests on several core principles:
- Psychological problems are often based on faulty or unhelpful ways of thinking.
- Problems can be improved by targeting thoughts and perceptions.
- Individuals can learn to evaluate thoughts rationally and respond to challenges in a more adaptive manner.
The underlying concept is that your thoughts, behaviors, emotions, and physical sensations all interconnect. Instead of focusing on past causes, CBT looks at present problems and how to change them.
The goal of CBT is to help you identify harmful thought and behavior patterns and acquire the tools to adopt more realistic, helpful mindsets and responses. This allows you to cope better with life’s challenges.
How Does Cognitive Behavioral Therapy Work?

CBT aims to improve mental health by equipping clients with skills to modify dysfunctional thoughts, emotions and behaviors. Treatment generally involves these core components:
Identifying Problematic Thoughts and Behaviors
The first step is to recognize unhelpful thoughts and actions that negatively influence emotions. Common techniques include keeping a journal and conducting behavioral experiments. For example, if you feel anxious at work, you would track associated automatic negative thoughts and behaviors.
Linking Thoughts and Feelings
Next, you look at connections between thoughts, feelings and behaviors. Negative thoughts often precipitate distressed emotions. And behaviors can be reactions to those thoughts and feelings. Recognizing these connections is key.
Evaluating Thoughts
You also learn to analyze thoughts rationally and objectively. Key questions include: Is this thought realistic? Is there another way to view this? What evidence disputes this idea? This helps reveal distorted thinking.
Alter Unrealistic Thinking
You practice reshaping negative thoughts into more realistic, alternative thoughts. This could involve examining evidence that contradicts a threatening belief.
Apply New Thinking
Next, you begin intentionally replacing unhelpful thoughts with more honest, realistic ones through repetition and practice. The goal is to make this new thinking a habit.
Change Behaviors
You also develop skills to change behaviors by practicing them. This might involveexposure activities or behavioral experiments to test fearful predictions. Facing fears provides real-world experiences that disprove false beliefs.
CBT therapists provide education, guidance and support in this process. But you must play an active daily role practicing new skills for lasting improvement. It takes consistent work inside and outside of sessions.
Cognitive Distortions Targeted by CBT

Cognitive distortions are irrational or exaggerated ways of thinking that warp perceptions. CBT helps identify and challenge cognitive distortions like these:
- All-or-nothing thinking – Viewing situations in absolute, black and white terms. For example, “If I’m not perfect, I’m a total failure.”
- Catastrophizing – Automatically expecting the worst possible outcome. For instance, “I know this presentation will be a disaster.”
- Disqualifying/Discounting the positive – Unfairly dismissing positive facts or focusing on negatives. For example, “I got the job, but it was just luck.”
- Emotional reasoning – Basing conclusions solely on feelings, rather than facts. For instance, “I feel anxious, so I must be in danger.”
- Jumping to conclusions – Making assumptions not grounded in facts. For example, “My partner is upset, they must not love me.”
- Labeling – Broadly characterizing people or events with negative words. Such as calling oneself a “loser” for making a mistake.
- Magnification/Minimization – Exaggerating negatives or shrinking positives. “She hasn’t called all day – our relationship must be over.”
- Mental filter – Only dwelling on the negative and ignoring the positive. For instance, “My presentation bombed” (ignoring praise received).
- Mind reading – Assuming you know what others are thinking, without evidence. For example, “My boss thinks I’m incompetent.”
- Overgeneralization – Broadly applying conclusions from a single event. Such as “I didn’t get that job, so I’ll never get a job I really want.”
- Personalization – Unfairly blaming yourself for external events. Like thinking a friend didn’t return your call because you did something wrong.
- “Should” statements – Criticizing yourself or others with “shoulds”, “musts”, “oughts” and “have tos.” For instance, “I should never make mistakes.”
- Tunnel vision – Only seeing negatives in a situation. For example, “My partner cheated on me – our whole relationship was a lie.”
Learning to identify and re-frame distorted thinking patterns is a pivotal part of CBT.
Cognitive Restructuring for Anxiety
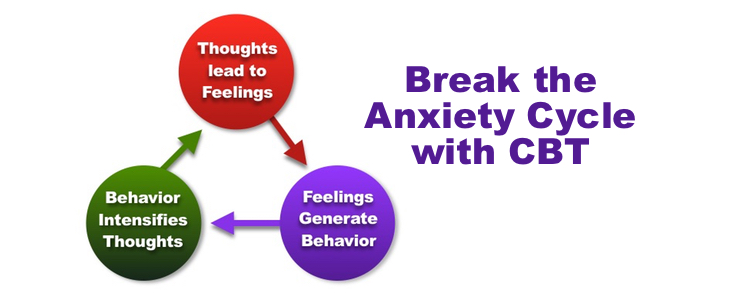
Cognitive restructuring is a core CBT technique that involves identifying negative automatic thoughts that trigger anxiety and replacing them with more realistic alternative thoughts.
For example, imagine you’re anxious about an upcoming work presentation. You may have an automatic thought like “I’m going to mess up and look so stupid.” CBT helps you reframe the thought to something more realistic, like “I always get nervous before presenting, but I’ve done fine in the past. I know this topic and have prepared.”
Restructuring involves these evidence-based steps:
- Identify automatic negative thoughts – What distressed you and what thought popped up?
- Examine for cognitive distortions – Is the thought exaggerated or irrational? If so, how?
- Challenge the thought’s validity – What evidence disputes it? What alternative views exist?
- Develop a rational response – How could you reframe the thought to be more fair and realistic?
- Replace the distorted thought – Consciously swap in the new thought.
With practice, this process allows you to catch and dispute unhelpful thoughts before anxiety escalates. Over time, rational thinking becomes more automatic.
Common CBT Techniques and Tools
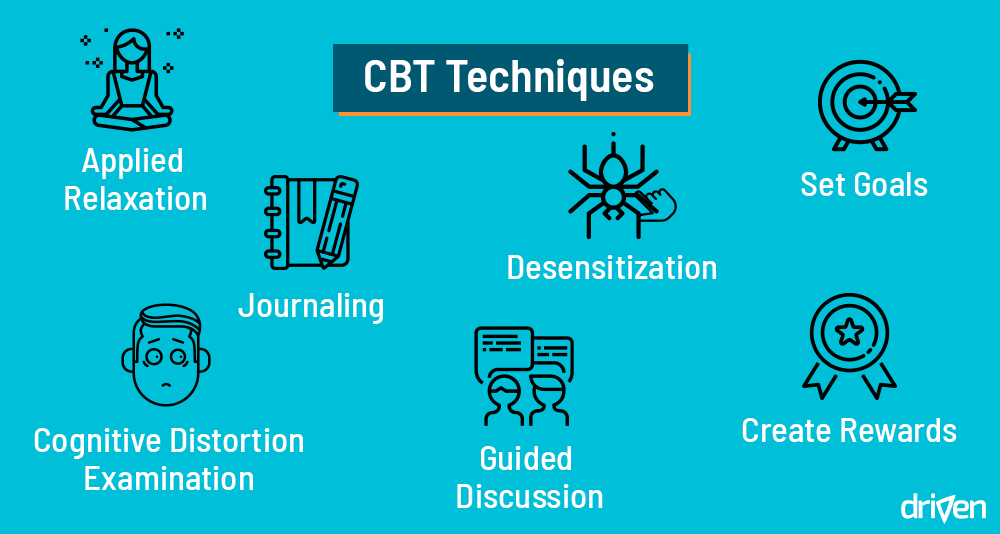
CBT uses a variety of techniques and tools to identify problematic thoughts/behaviors and develop new skills. Common methods include:
Goal Setting
You collaboratively define treatment goals and steps to achieve them. Progress is tracked weekly. This provides a sense of direction and accomplishment.
Homework
You practice applying skills learned on your own through reading assignments, self-monitoring, reflection activities and behavioral exercises. This extends learning beyond sessions.
Role Playing
You act out challenging situations with the therapist or in groups. This lets you practice skills in a safe environment. Feedback helps fine-tune responses.
Modeling
The therapist demonstrates effective skills, thoughts and behaviors in sessions that you can mimic. Watching a model helps teach new ways of interacting.
Journaling
Writing about thoughts, feelings and behaviors related to problems helps raise awareness of unhelpful patterns. Journaling can track progress too.
Socratic Questioning
Therapists ask carefully crafted questions to prompt realizations, illuminate irrational beliefs and encourage self-reflection. This indirect approach avoids debate.
Behavioral Experiments
You test out feared predictions to see if they come true and conduct other challenges to disprove negative beliefs through real-world experiences.
Exposure Therapy
You gradually confront anxieties in a structured, therapeutic setting to extinguish associated fear and anxiety. This teaches fears are manageable.
Cognitive Restructuring
You learn to identify and dispute irrational or exaggerated thoughts and replace them with more realistic, positive self-talk through reason and evidence.
Problem-Solving
You break problems into smaller parts, brainstorm solutions, evaluate options and develop plans to take constructive action rather than avoiding issues.
Relaxation Techniques
Deep breathing, visualization, mindfulness and progressive muscle relaxation help relieve anxiety and stress and provide tools to regulate emotions.
Emotion Regulation
Skills like identifying and labeling feelings, expressing emotions adaptively and modifying reactions help manage overwhelming or difficult emotions.
Communication Skills
You learn assertive communication techniques like using “I feel” statements, active listening and compromise to improve relationships.
Effectiveness of CBT for Mental Health

Hundreds of studies demonstrate CBT is highly effective for a wide range of mental health concerns. It’s considered a best practice treatment for:
- Depression – CBT helps identify and challenge negative automatic thoughts fueling sadness. Behavioral activation also engages people in rewarding activities.
- Anxiety disorders – CBT teaches coping skills to manage symptoms and reduce avoidance. Exposure therapy also helps patients face fears.
- Eating disorders – CBT focuses on body image, underlying beliefs and behaviors around eating, purging, exercise, etc.
- Substance abuse – CBT helps people recognize risky situations, improve coping skills and change social support and behaviors.
- Bipolar disorder – CBT aids with emotion regulation and addresses dysfunctional thoughts that arise during mood episodes.
- Schizophrenia – CBT focuses on improving community functioning by teaching coping and social skills to manage symptoms.
- Insomnia – CBT-I helps identify and change thoughts, behaviors and habits contributing to sleep problems.
- Relationship issues – CBT improves communication, problem-solving, cognitive distortions and behaviors affecting relationships.
- Anger management – CBT increases emotional awareness and regulation and dispute irrational thoughts triggering anger.
- Chronic pain – CBT teaches coping techniques like pacing, relaxation and challenging unhelpful pain beliefs.
CBT blends well with medications and helps prevent relapse after treatment too. It provides long-term skills rather than being a “quick fix.” Research confirms CBT’s effectiveness for both mood and behavioral disorders.
CBT Interventions
/cdn.vox-cdn.com/uploads/chorus_image/image/70159160/GettyImages_1324376942.0.jpg)
CBT clinicians draw from a variety of interventions and select techniques to meet individual needs. Common interventions include:
Cognitive Restructuring
Identifying and reframing exaggerated or irrational thoughts is pivotal to CBT. You learn to challenge negative self-talk and replace it with more realistic perspectives.
Exposure Therapy
Controlled, gradual exposure to fears helps safely disprove overestimations of threat. Examples include confronting social anxiety triggers or touching contaminated objects for OCD.
Behavioral Activation
Encouraging involvement in pleasurable, rewarding activities boosts mood and reduces avoidance in depression. Scheduling activities and tracking mastery helps.
Anxiety Management Skills
CBT teaches anxiety coping strategies like abdominal breathing, progressive muscle relaxation, visualization and mindfulness meditation.
Problem-Solving
Breaking down problems, listing solutions, weighing pros and cons of options and developing action plans helps resolve issues directly.
Assertiveness Training
Learning assertive communication, emotion regulation and conflict resolution skills helps build confidence and balance relationships.
Sleep Hygiene
Following routines and habits that promote restful sleep, like limiting electronics before bed, improves sleep problems.
Emotion Regulation Skills
Identifying, labeling, expressing and modifying emotions provides healthy strategies to handle challenging feelings. This lowers emotional reactivity.
Mindfulness-Based CBT
Mindfulness meditation helps patients observe thoughts non-judgmentally, increase present focus, reduce rumination and manage cravings.
Behavioral Experiments
Doing activities to test out feared beliefs in real life disproves irrational fears and stops avoidance.
CBT clinicians mix and match appropriate techniques to meet treatment goals. Integrating interventions is collaborative based on individual needs.
Types of Cognitive Behavioral Therapy
Many CBT variants exist for specific concerns. While techniques differ, the core principles remain the same. Some common types of CBT include:
- Cognitive Therapy (CT) – Developed by Aaron Beck, CT focuses mainly on identifying and changing distorted thinking.
- Rational Emotive Behavior Therapy (REBT) – Created by Albert Ellis, REBT helps patients reshape irrational philosophies creating dysfunction.
- Dialectical Behavior Therapy (DBT) – DBT balances change and acceptance strategies. It treats borderline personality disorder.
- CBT-Insomnia (CBT-I) – CBT-I targets thoughts and behaviors impeding sleep through sleep restriction, stimulus control, relaxation and cognitive techniques.
- Exposure Therapy – Also called prolonged exposure (PE), this CBT variant gradually exposes patients to fears to reduce anxiety/avoidance.
- Acceptance and Commitment Therapy (ACT) – ACT focuses on accepting unpleasant thoughts and committing to value-driven actions.
- Functional Analytic Psychotherapy (FAP) – FAP aims to improve personality disorders by providing therapists’ direct feedback during sessions.
- Behavior Therapy – This traditional form of CBT uses principles of classical and operant conditioning to change behaviors.
- Cognitive Processing Therapy (CPT) – CPT is used to treat post-traumatic stress disorder by reframing distressing thoughts about the trauma.
- Dialectical Behavior Therapy (DBT) – DBT balances change and acceptance strategies. It treats borderline personality disorder.
Tailored CBT programs also exist for concerns like anger management, chronic pain, OCD, bipolar disorder, schizophrenia, substance abuse, eating disorders and more.
Cognitive Behavioral Therapy Techniques
CBT practitioners employ a diverse range of techniques and tools to assess problems, teach coping skills, challenge unhelpful thinking and support behavior change. Commonly used practical CBT techniques include:
Goal Setting
The therapist and client collaborate to identify specific, measurable goals to work towards based on presenting concerns. Progress is tracked and goals evolve during treatment.
Homework Assignments
Homework extends skills learned in session through reading materials, self-monitoring, reflection activities, behavioral challenges and more completed between appointments.
Journaling
Writing exercises help clients log and reflect on thoughts, feelings, behaviors, progress, reactions to challenges and skill use related to targeted problems.
Socratic Questioning
Therapists mindfully ask probing questions to promote insight, reveal irrational thinking, explore alternatives, evaluate consequences and spark internal motivation to change.
Roleplaying
Practicing situations during sessions provides a safe space to build skills through mimicking reactions, testing out new responses and receiving coaching and feedback.
Modeling
Observing the therapist demonstrate effective examples of thoughts, behaviors, communication skills and emotion regulation during sessions helps teach clients new ways of interacting.
Behavioral Experiments
In vivo exposure assignments test feared beliefs through real world experiences to build coping skills and resilience.
Worry Postponement
Delaying worrying provides concrete proof worry can be managed and diffuses anxiety. Clients schedule short “worry periods” rather than ruminating all day.
Activity Scheduling
Clients build mastery by planning meaningful, enjoyable activities balanced with obligations into daily/weekly schedules. Activity logs track participation and mood.
Imagery
Visualization techniques like imagining handling situations adaptively or picturing anxious scenes until they no longer provoke anxiety can alter emotions/behavior.
Cognitive Restructuring
Identifying and replacing distorted thoughts with realistic perspectives shifts unhelpful beliefs fueling emotional distress and dysfunction.
Problem-solving
Breaking problems into parts, brainstorming solutions, weighing pros and cons of options and formulating action plans helps approach problems directly.
Relaxation Techniques
Diaphragmatic breathing, progressive muscle relaxation, guided imagery, mindfulness and other methods manage anxiety, improve sleep, and increase focus.
CBT clinicians mix and match appropriate techniques to meet individual needs and treatment goals collaboratively.
How Many CBT Sessions Are Needed?

The number of CBT sessions required depends on several factors:
- Type and severity of problems – More complex or longstanding issues typically need more sessions. For example, 40-60 sessions may be recommended for personality disorders and chronic depression versus 6-10 sessions for mild anxiety or depression.
- Individual needs and engagement – The pace of progress and how well you apply skills between sessions impacts length of therapy. Doing “homework” extends learning.
- Treatment setting – Settings with time limitations like employee assistance programs or college counseling centers may restrict sessions to 6-12.
- Therapeutic approach – The type of CBT modality used affects duration. Traditional CBT often involves 6-20 sessions. But newer acceptance-based approaches work faster.
- Frequency of appointments – Meeting weekly instead of every other week will naturally shorten the length of therapy.
- Insurance coverage – Policies often limit sessions based on diagnosis. Plans may approve 6-8 sessions initially and require approval for more.
- Budget and logistics – Practical factors like cost per session and scheduling availability can influence session limits too.
In general, research shows 8-12 weekly sessions of CBT for conditions like depression and anxiety can yield significant improvement for most people. More complex issues require longer-term treatment of usually 6 months or more.
How to Get the Most out of CBT

CBT requires consistent practice between sessions for optimal results. Here are helpful tips to maximize gains from CBT:
- Be an active participant – Speak up about your needs, offer feedback, ask questions, and discuss any difficulties about the therapy process. The more engaged you are, the more you’ll get out of sessions.
- Identify specific target problems – Developing concrete goals you want to accomplish makes progress easier to gauge. Vague goals like “feel happier” are hard to measure.
- Do homework – Practice and repetition is key for learning new skills. Doing reading assignments, self-monitoring, worksheets and activities outside of sessions reinforces new tools.
- Keep an open mind – For CBT to work, you must be willing to consider new perspectives and experiment with unfamiliar techniques. Being defensive about old habits sabotages progress.
- Share all relevant information – Providing details about symptoms, thoughts, behaviors, stressors, and lifestyle aids therapists in tailoring treatment. But don’t feel pressured to disclose more than you’re ready to.
- Monitor thoughts, feelings and behaviors – Paying close attention to internal experiences and reactions provides data to identify patterns to target in therapy. Tracking progress in a journal accelerates insights.
- Practice outside of session – Consistently applying CBT skills in everyday life embeds learning and builds confidence using techniques independently. This takes repetition over time.
- Be patient with the process – CBT takes consistent practice over weeks or months to see results. Don’t be discouraged if change does not come quickly. Progress often comes in small steps. But it adds up.
- Communicate about any blocks – Challenges like negative self-talk undermining efforts or difficulty motivating to use skills should be addressed. Your therapist can help strategize solutions.
- Schedule post-treatment booster sessions – Periodic CBT tune-up sessions prevent relapse and help squash resurfacing of old patterns. Many therapists recommend this.
- Remember recovery takes work – CBT provides tools, but you must use them. Effort invested directly impacts outcomes. Be kind, but keep pushing yourself. You’re worth it!
Actively participating, closely tracking your experiences, and rehearsing CBT skills builds up vital mental muscle memory over time. Think long-term progress through commitment.
CBT Worksheets, Techniques and Handouts
CBT worksheets, handouts, audio/video and other resources help bring concepts to life. Therapists often provide materials for reference outside of sessions. Helpful CBT tools include:
CBT Thought Records – These forms walk you through documenting upsetting situations, associated thoughts/feelings, analyzing and reframing irrational thinking, and rating intensity of emotions before and after restructuring unhelpful thoughts.
CBT Thought Challenging Worksheets – These worksheets use prompts and questions to teach core thought challenging techniques like examining evidence for and against distressing thoughts.
CBT Worry Postponement Logs – These logs help diffuse anxiety about worries through scheduling short dedicated “worry periods” rather than ruminating endlessly.
CBT Behavioral Activation Activity Scheduling – These forms aid depressed clients in planning and tracking participation in enjoyable, productive activities balanced with obligations.
CBT Goal Setting Worksheets – These worksheets help break big goals into smaller, manageable steps and track incremental progress. Having realistic timeframes keeps motivation up.
CBT Journaling – Writing reflectively about automatic thoughts, cognitive distortions, upsetting events, progress, etc. builds self-awareness and tracking patterns.
CBT Coping Cards – Handy pocket-sized cards record personalized coping strategies and positive statements to reference when distressed instead of resorting to unhelpful habits.
CBT Education Handouts – These handouts summarize CBT concepts like common cognitive distortion, fight or flight response, and relaxation techniques for clients to reference later.
CBT Thought Records App – This popular app conveniently allows you to log, categorize and chart thought records between sessions.
Tailored CBT worksheets distill concepts and supplement sessions. Therapists may create materials or provide research-validated handouts.
CBT for Depression
-for-Depression.jpg)
CBT is highly effective for treating depression. The approach helps identify and reframe negative automatic thoughts and self-defeating behaviors that maintain depressed moods. Common CBT techniques for depression include:
Cognitive Restructuring
Identifying and challenging pessimistic thoughts is pivotal to lifting depression. You learn to reframe distorted thinking patterns like negative predictions, perfectionism and catastrophizing.
Behavioral Activation
Since depression often leads to isolating and withdrawing from fulfilling activities, therapists help schedule pleasurable, rewarding actions balanced with obligations. This boosts mood through accomplishment.
Problem-Solving
Breaking problems down into smaller parts, brainstorming solutions, weighing pros and cons of options, and creating action plans helps take constructive steps despite depressed feelings.
Relaxation Techniques
Learning relaxation skills like controlled breathing, progressive muscle relaxation, visualization and mindfulness meditation helps calm the body to reduce fatigue, improve sleep and lower anxiety.
Positive Activities
Recording daily positive thoughts, writing gratitude lists, performing small acts of kindness, and doing one fun activity per day reinforces positive thinking and actions.
Sleep Hygiene
Regulating sleep patterns, limiting naps, and following routines to promote restful sleep improves fatigue and concentration. Adequate sleep reduces depression risk.
Research confirms CBT is a leading therapy choice for depression, either combined with antidepressant medication or individually. The skills you learn can strengthen resilience beyond the treatment period too.
Group CBT Therapy

While most CBT is delivered one-on-one, a group therapy format offers unique benefits like these:
- Peer support – Members encourage each other and often exchange contact information to provide support outside group. Knowing you’re not alone is reassuring.
- Vicarious learning – Observing others model skills and share experiences provides examples to follow. This accelerates learning.
- Shared experiences – Hearing how other members interpret situations provides fresh perspectives you may relate to.
- Social skills practice – The group setting allows members to practice socialization skills in a safe environment under a therapist’s guidance.
- Extended practice – More time is available to practice CBT techniques like roleplaying, modeling, problem-solving and social skills through activities.
- Cost-effectiveness – Sharing one therapist’s time among several people reduces costs compared to individual therapy.
Of course, the downside is less personalized attention from the therapist. But the mix of support, shared understanding, and observing others often offsets this drawback. Overall, research shows group CBT is just as effective as individual CBT for many common issues like depression, anxiety, and eating disorders.
Online CBT Therapy

Receiving CBT through online programs, videoconferencing, messaging and apps is known as internet-delivered CBT or iCBT. This format has expanded access to CBT. Benefits include:
- Convenience – Online CBT allows you to participate anywhere, anytime by removing geographic and scheduling barriers.
- Privacy – The anonymity of online settings may help those hesitant about in-person therapy feel more comfortable sharing and engaging.
- Continual access – Having CBT resources available 24/7 via apps or recorded sessions allows you to revisit materials as needed.
- Flexible pacing – You can review lessons or practice techniques at your own speed instead of waiting for weekly appointments.
- Cost – Online CBT is often more affordable than traditional in-office therapy.
- Accessibility – Online options help those unable to regularly attend in-person sessions get quality mental healthcare.
Potential limitations are reduced personalization, reliance on motivation for self-directed learning, and lack of body language cues during video sessions. Overall, research confirms iCBT programs are clinically effective and have high patient satisfaction. Many therapists now blend online tools with traditional sessions too.
CBT Certification and Training
![5 Best CBT Training Courses - [OCT 2023]](https://s3.amazonaws.com/coursesity-blog/2021/09/Cognitive_behavioural_therapy.png)
There are several paths to become trained in CBT depending on your counseling degree and career stage:
- Graduate degree – Most graduate programs in clinical psychology, counseling, and social work offer courses in CBT models and techniques as part of the core curriculum. Internships also provide clinical training experience delivering CBT.
- Post-graduate training – After graduation, you can complete a postdoc, fellowship or formal training program focused on immersive CBT clinical practice, research, supervision and advanced credentialing.
- Workshop-based training – Various continuing education institutions and professional organizations offer multi-day intensive CBT skills workshops for practicing clinicians looking to expand their repertoire. Workshops range from two days to two weeks typically.
- Online training – For flexibility, many therapists take individual CBT skills courses virtually through platforms like the Beck Institute, E-learning CBT, and the Association for Behavioral and Cognitive Therapies or get an online Certificate in CBT.
- Certification – Several organizations like the National Association of Cognitive-Behavioral Therapists offer certifications after therapists demonstrate completion of accredited CBT training, supervised experience, and an exam. Certification often requires continuing education too.
Investing in ongoing CBT training allows clinicians to stay up-to-date with the latest techniques and applications to improve their therapy skills.
How to Become a Cognitive Behavioral Therapist

Becoming a skilled CBT therapist involves education, clinical training and credentialing:
- Earn a master’s degree – Complete a Master’s in Counseling, Psychology, or Social Work from an accredited graduate program. Core coursework provides foundation in human development, ethics, assessment, counseling skills and theoretical approaches.
- Pursue CBT coursework & training – Take all CBT electives possible. Seek a practicum and internship site that uses CBT. Attend CBT workshops and conferences. Consider a CBT graduate certificate or postdoc training.
- Get supervised clinical hours – Accrue required clinical hours and pass licensing exams for your state. Exposure to CBT during trainee hours is ideal. Obtaining credentials like LPC (Licensed Professional Counselor) demonstrates qualifications.
- Consider CBT certification – Getting certified by the National Association of Cognitive-Behavioral Therapists, Academy of Cognitive Therapy, or Beck Institute demonstrates specialized expertise.
- Get experience – Seek employment at practices specializing in CBT. Having CBT referenced on your resume helps land positions too. Gain skills presenting on CBT topics.
- Maintain credentials – Keep up-to-date with CBT advances through continuing education. Ongoing training improves competency. Renew certifications as needed.
With dedication to education and experience, therapists interested in CBT can gain expertise in delivering this gold-standard approach either as general practice or a specialty area.
Choosing a CBT Therapist

Finding a competent CBT therapist is key to getting quality treatment. Here are tips for choosing a practitioner:
- Verify licenses – Check credentials like Licenced Clinical Social Worker (LCSW) or Licensed Professional Counselor (LPC) showing proper training and passing of exams.
- Look for CBT experience – Search for CBT, cognitive therapy, or dialectical behavior therapy on the therapist’s psychologytoday profile or website to confirm expertise. Or request their CBT training background.
- Ask about specialization – Inquire what specific CBT therapies they practice like exposure therapy, sleep CBT, anger management, etc. Experience treating your concerns is ideal.
- Consider credentials – Voluntary certifications like those from the National Association of Cognitive-Behavioral Therapists indicate substantial specialized training.
- Request a consultation – Have a brief free phone call to ask questions and explain your reasons for seeking CBT before scheduling. Get a sense if your personalities may fit.
- Verify insurance coverage – If using insurance benefits, confirm the provider accepts your plan and that your diagnosis is covered before starting sessions.
- Compare cost – Ask fees upfront so you can anticipate costs and shop rates if needed. Many offer sliding scale options.
With some research, you can find an accredited, experienced CBT therapist well-suited to help you meet your mental health goals and improve coping.
Frequently Asked Questions About CBT
What’s the difference between CBT and talk therapy?
While CBT contains talking just like traditional talk therapies, the key difference is CBT takes a more active, strategic approach. The therapist and client collaborate to set goals, analyze thinking and behavior patterns, develop coping skills and directly address problematic symptoms using evidence-based techniques. CBT focuses on the “here and now” while talk therapy typically explores the past more.
Does CBT really work?
Yes, decades of clinical research support CBT as an effective therapy for a wide range of mental health issues. It equals or surpasses other therapeutic approaches for problems like depression, anxiety, eating disorders, and substance use based on symptom improvement, recovery rates, and relapse prevention. CBT provides clients with practical tools to manage challenges long term.
Is CBT better than medication?
CBT and psychiatric medication are equally effective for many conditions like moderate depression or anxiety. But studies show combining CBT and medication works best for more severe cases since therapy gives you skills to manage recurrences. CBT also has lower relapse rates than medication alone after finishing treatment in many studies. But medications may be needed to help moderate symptoms initially. CBT and medication complement each other.
Does insurance cover CBT?
Most insurance plans cover some amount of CBT because of its established efficacy. But coverage and session limits depend on your diagnosis and plan. Many plans require prior authorization after initial visits. Check your benefits. CBT is considered out-of-network for plans using managed care systems. Sliding scale options can offset out-of-pocket costs.
Is online CBT effective?
Yes, several studies confirm online CBT programs produce equivalent results as face-to-face CBT for many common conditions like depression, anxiety, OCD and insomnia. More severe cases still benefit from blended care with some face-to-face sessions. Benefits of online CBT include lower cost, flexibility and accessibility. Leading agencies like the British Association for Behavioural and Cognitive Psychotherapies endorse properly designed iCBT’s efficacy.
How much does CBT cost?
CBT costs vary based on location, provider degrees, and insurance coverage but range between $75-$250+ per 50-minute session. Online CBT programs tend to cost $35-$70 monthly. CBT is cost-effective because it produces durable results faster than other open-ended therapies. Many therapists offer reduced sliding scale fees too.
This comprehensive guide provided a research-backed overview explaining what CBT is, how it helps, who it can benefit, techniques used, session frequency, training options and helpful advice to get the most from cognitive behavioral therapy. CBT equips people with practical tools to improve coping, resilience and mental health through a present-focused, goal-oriented process.




















.jpg)





/cdn.vox-cdn.com/uploads/chorus_image/image/70159160/GettyImages_1324376942.0.jpg)


-for-Depression.jpg)


![5 Best CBT Training Courses - [OCT 2023]](https://s3.amazonaws.com/coursesity-blog/2021/09/Cognitive_behavioural_therapy.png)

