What is Reactive Attachment Disorder?

Reactive attachment disorder (RAD) is a rare but serious condition that affects a child’s ability to form emotional bonds with their primary caregivers. RAD stems from neglect, abuse, or other trauma during the first few years of life. Children with RAD have difficulty trusting caregivers and struggle to feel secure, even when cared for in a loving home. They may act out, withdraw, or engage in dangerous behaviors.
With treatment, kids with reactive attachment disorder can develop healthier attachments. The earlier it’s caught, the better the outcome. But without intervention, RAD can have lifelong consequences for relationships, self-image, and even physical and mental health.
What Causes Reactive Attachment Disorder?

Reactive attachment disorder arises from extremely disrupted care during infancy and toddlerhood. Causes include:
- Repeated changes in primary caregivers, such as multiple foster placements
- Physical, emotional, or sexual abuse from caregivers
- Neglect—leaving a child’s physical and emotional needs unmet
- A lack of interaction from adult caregivers
Young children need consistent, nurturing care to thrive. If loving, reliable relationships are absent, children can’t form healthy attachments. Their brain development is disrupted. This lays the groundwork for attachment disorders.
RAD isn’t caused by temperament alone. But children with challenging temperaments may especially rely on sensitive caregiving to soothe and comfort them. Without that, they’re at risk for attachment issues.
Reactive Attachment Disorder Symptoms
:max_bytes(150000):strip_icc()/what-is-an-attachment-disorder-4580038_FINAL22-a5fcad506fa6456d88c35fa6d316afb7.jpg)
Reactive attachment disorder can take two forms:
Inhibited type. With the inhibited type of reactive attachment disorder, children are extremely withdrawn, disconnected, and resistant to comfort—even from caregivers they’re familiar with. Symptoms of the inhibited type include:
- Avoiding eye contact or physical contact
- Refusing comfort even when hurt, afraid, or sad
- Failing to seek care or respond when caregivers are present (“freeze response”)
- Resisting social interactions
- Appearing disconnected, distant, or numb
Disinhibited type. The disinhibited type of reactive attachment disorder results in overly familiar, indiscriminate behavior even with strangers. Symptoms of the disinhibited type include:
- Seeking comfort from strangers rather than caregivers (“indiscriminate friendliness”)
- Willingness to go off with strangers with little or no hesitation
- Difficulty complying with requests or rules (“defiance”)
- Appearing clingy, attention seeking, or hyperactive
Keep in mind that many reactive attachment disorder symptoms overlap with other conditions like autism spectrum disorder, attention deficit hyperactivity disorder (ADHD), and more. See your doctor if you notice any of these red flags.
When to Seek Help for Reactive Attachment Disorder

The earlier reactive attachment disorder is addressed, the better the outcome. Left untreated, RAD can have lifelong consequences. Seek help from your pediatrician or a child mental health professional if your child:
- Rarely seeks comfort or responds to nurturing from caregivers
- Doesn’t seem attached to anyone specific—even you
- Is extremely controlling, defiant, clingy, or doesn’t acknowledge typical social boundaries
- Takes excessive risks or is dangerously impulsive
- Lacks cause and effect thinking
- Has delayed speech, learning, or motor skills
Keep in mind that some reactive attachment disorder behaviors—like avoidance or resistance—emerge as coping strategies. Kids aren’t choosing to disconnect. Get support right away to help your child develop trust and feel safe.
Getting a Reactive Attachment Disorder Diagnosis

Since there are no lab tests for reactive attachment disorder, diagnosis relies on observation of symptoms and interactions with caregivers. It’s best done by a clinical psychologist, psychiatrist, social worker, or other mental health professional with attachment disorder expertise.
To make a RAD diagnosis, providers will:
- Interview you, teachers, and other caregivers about your child’s relational and behavioral history
- Directly observe your child’s social and emotional functioning, especially with caregivers
- Rule out or account for conditions like autism spectrum disorder, intellectual disabilities, and more
Reactive attachment disorder is a serious diagnosis. Your provider will want to be very sure before diagnosing RAD. Be prepared to spend multiple sessions providing background. The more info you can share, the better.
Types of Reactive Attachment Disorder Treatment

Treatment for reactive attachment disorder aims to help kids:
- Develop trust and feel secure with caregivers
- Learn healthy emotional regulation and self-soothing skills
- Understand social boundaries and expectations
- Process trauma safely under a therapist’s guidance
A comprehensive treatment approach often includes:
1. Attachment-based therapy. This directly focuses on strengthening the caregiver-child bond through play, appropriate physical contact, emotional attunement, andempathy. Examples include dyadic developmental psychotherapy, Filial Therapy, and Theraplay.
2. Trauma-focused psychotherapy. EMDR, somatic therapy, and trauma-focused cognitive behavioral therapy help kids safely process past trauma. This is critical for developing new trust.
3. Caregiver education. Helping parents and caregivers understand RAD and learn emotional regulation techniques sets everyone up for success.
4. In-home support. Strategies like trust-based relay modeling equip all caregivers to interact in consistent, therapeutic ways.
5. Parent-child interaction therapy (PCIT). With coaching from a therapist, PCIT uses “bug-in-ear” technology to guide caregiver responses in real time as they play with their child. This helps build patterns of healthy attachment.
6. Residential treatment. If issues are severe enough to require 24/7 clinical support, residential facilities provide attachment-based care and psychotherapy.
Medication is not used to treat reactive attachment disorder itself. But it can sometimes help manage related conditions like anxiety, depression orADHD symptoms.
Improving Relationships with Reactive Attachment Disorder

No matter the specific treatment approach, caregivers play a pivotal role helping kids with reactive attachment disorder develop healthyer bonds. With support and practice, you can learn to:
- Provide soothing physical contact and nurturing care, even if your child resists or avoids it. Be patient, responsive, and emotionally available.
- Stick to routines and consistent emotional responses. Kids with RAD rely on predictability.
- Use simple language and deliver praise and constructive criticism calmly. Limit yelling or harsh reactions.
- Set clear boundaries and reinforce positive social skills. But keep requests simple.
- Take care of yourself! Managing your own stress empowers you to meet your child’s extra needs.
It’s heartbreaking when your love and care don’t come through for your child. With time, consistency, and professional help, you can get through it together.
Coping with Reactive Attachment Disorder at Home

Kids with reactive attachment disorder often lack some basic living skills when it comes to hygiene, self-control, and more. You can encourage healthy habits with structure, routine, patience, and praise. Useful strategies include:
Schedule – Make daily routines predictable but flexible enough to meet sensory needs. Use pictures, charts, or visual timers.
Prevent power struggles – Give choices (“Do you want to brush your teeth before or after bath time?”) but not too many. Use neutral language.
Teach coping skills – Help your child identify emotions and de-escalate meltdowns. Have calming activities ready to use.
Get moving – Have a park trip, family yoga session, or dance party to work out wiggles. Physical play relieves stress.
Unplug – Limit screen time. Encourage hands-on play, household tasks, crafts and reading together instead.
Connect regularly – Set aside special one-on-one time each day. Even a short, attentive chat helps build attachment.
Keep it positive – Notice good behavior often. Prevent problems before they start. Save discipline as a last resort.
Stay patient! It takes time and consistency. But supporting development at home is so important for overcoming RAD.
Reactive Attachment Disorder in Older Children & Teens

While reactive attachment disorder is considered a disorder of infancy and childhood, impacts often persist through the teen years. As kids get older, RAD can manifest in ways like:
- Physical or verbal aggression
- Lying, stealing, and other delinquent behaviors
- Running away or skipping school
- Risky sexual activity
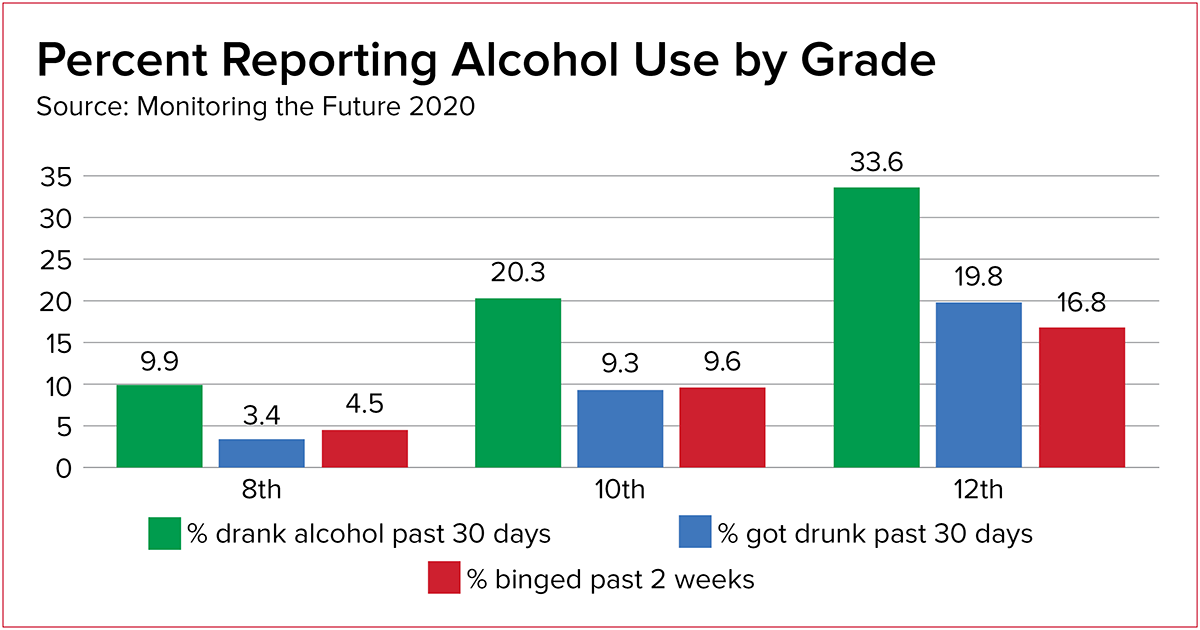
- Alcohol or drug use
- Self-harm
The brain becomes less plastic over time. So reactive attachment disorder can become more ingrained. But it’s never too late to intervene. Intensive psychotherapy and family therapy provides older kids the support they need for healthier relationships.
Hope for Overcoming Reactive Attachment Disorder
If caught early, kids with reactive attachment disorder often improve greatly with prompt treatment. But even older children and teens can overcome RAD’s impacts with time and consistency.
Healing happens step-by-step. Stay focused on the progress your child is making, not just the challenges ahead. And take care of yourself along the way. Managing your own stress empowers you to meet their extra needs with sensitivity and care.
With family support, professional treatment tailored to your child’s needs, and most of all—patience and love—healing is absolutely possible. If you suspect reactive attachment disorder, reach out now. Don’t lose hope. Help is available.
Finding the Right Therapist for Reactive Attachment Disorder

Getting the right therapy is key to successfully treating reactive attachment disorder. Look for a provider with extensive experience working with attachment issues. Key things to look for include:
- Advanced training in attachment-based therapies like Dyadic Developmental Psychotherapy (DDP), Theraplay, or Parent-Child Interaction Therapy (PCIT). These directly address attachment difficulties.
- Knowledge of trauma-informed care. A background in EMDR, somatic therapy, or similar helps kids process past trauma safely.
- Flexible therapeutic styles. Play therapy, experiential techniques, and family sessions are often more engaging for kids than just talk therapy.
- Ongoing education. Attachment therapy is a newer, evolving field. Look for commitment to the latest training.
- Support for caregivers. The best therapists empower you with education and equip you to respond sensitively.
- Multidisciplinary teams. Psychologists, counselors, social workers, occupational therapists and others often collaborate for comprehensive care.
- Specialized experience with foster/adoptive families. Therapists who understand unique dynamics with RAD can better support your family.
Don’t underestimate the importance of personal fit, too. Look for a provider you and your child feel comfortable with. That rapport helps build trust essential to the process.
Finding Support for Reactive Attachment Disorder

In addition to professional treatment, connecting with others who understand reactive attachment disorder’s impacts can provide incredible support. Useful resources include:
- Online forums. Connecting with other RAD parents online provides tips and solidarity. But be mindful of avoiding “support” that promotes unhelpful attachment therapy techniques.
- In-person support groups. Look for meetups through your provider or local attachment disorder networks. Sharing stories in person is so valuable.
- Books. Memoirs like “The Connected Child” offer insights into daily life with RAD from parents who have been there.
- Articles and videos. Hear from attachment disorder experts and adults who overcame early relational trauma.
- Social media. Follow therapists and bloggers discussing healthy attachment strategies. Just be wary of misinformation.
- Advocacy organizations. Groups like Advocates for Children in Therapy promote ethics and education around attachment disorders.
Don’t underestimate your own inner strength either. This is so challenging, but you’ve got this. With support, you and your child can continue progressing together.
Boosting Developmental Skills with Reactive Attachment Disorder
In addition to attachment difficulties, reactive attachment disorder often delays other developmental milestones too. Kids may struggle with:
- Physical coordination
- Speech and language abilities
- Cognitive, learning, and memory deficits
- Poor impulse control and emotional regulation
- Difficulty understanding social cues
A comprehensive treatment approach promotes development across all domains. Useful strategies include:
- Occupational therapy to improve fine motor skills through playful activities
- Physical therapy for building gross motor coordination and strength
- Speech therapy targeting communication, listening, and oral motor abilities
- Cognitive behavioral therapy (CBT) to boost emotion management, memory, and social skills
- Social stories and role playing to practice appropriate behavior in different settings
- Assistive technology like picture charts, smart watches with timers and alerts, and more
- Testing for learning disorders and providing academic support tailored to your child’s needs
Don’t hesitate to bring up any developmental concerns with your child’s providers. Early intervention can help them gain important life skills.
Should You Adopt a Child with Reactive Attachment Disorder?

When considering adoption or foster placement, learning a child has reactive attachment disorder can feel concerning. But with preparation and access to treatment, RAM doesn’t have to stop you from welcoming a child into your heart and home.
It’s natural to have some fears. But don’t let worst case scenarios stop you. With structured support, most kids with reactive attachment disorder improve dramatically. Key tips include:
- Learn all you can about RAD before placement. Understand common issues and be ready to advocate for your child.
- Have a strong attachment-based treatment team lined up ahead of time. Consistency is critical.
- Prepare your family through attachment-focused parenting education. Get everyone on the same page.
- Set realistic expectations around timelines. Your child may not attach quickly. Have patience.
- Build your support network. Connect with other RAD adoptive and foster parents.
- Practice self-care. Get respite care when needed. Manage your own stress.
With preparation and access to care, a reactive attachment disorder diagnosis doesn’t have to delay welcoming a child in need into a loving “forever family.”
How to Discipline a Child with Reactive Attachment Disorder

For kids with reactive attachment disorder, typical discipline strategies often backfire. RAD makes it hard for children to internalize cause-and-effect thinking. And harsh punishments can retraumatize.
But through empathy, flexibility, and creativity, you can reinforce positive behavior. Useful tips include:
- Clearly explain rules and consequences in simple terms. Use visual aids if needed.
- Focus on rewards over punishments. Praise good behavior often. Provide small treats, special activities, chart-based rewards, etc.
- Pick your battles. Let minor things go to avoid power struggles. Redirect instead of reprimanding.
- Offer frequent empathy and emotional check-ins. See misbehavior as a sign your child needs connection.
- Provide sensory/movement breaks. Blowing bubbles, stretching, or listening to music helps reset.
- Give clear warnings before transitions. Use timers, social stories, and preview what’s next.
- Involve your child in solution finding. “What can we try next time instead of yelling?”
- Keep responses calm, consistent, and predictable. Your stability provides security.
It takes creativity and patience! But responsive, empathetic limit setting helps build new relational patterns.
How Trauma Impacts Brain Development
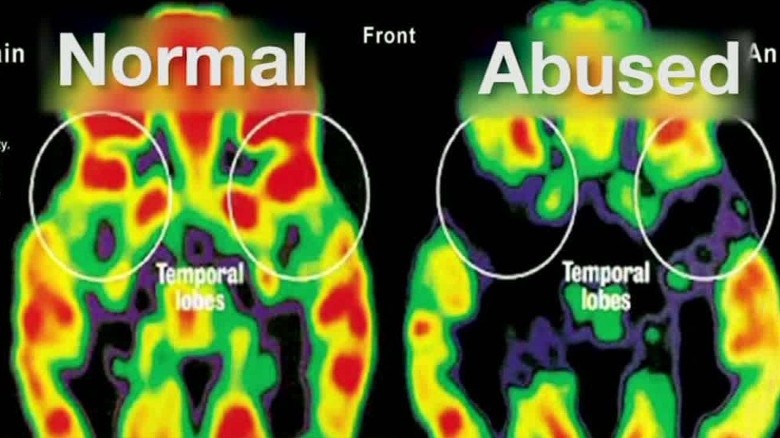
Trauma during infancy and childhood has profound impacts on brain development. Neuroimaging shows reactive attachment disorder literally changes brain structure and functioning.
Structural Changes
- Smaller cerebral and prefrontal cortex volumes
- Reduced connectivity between left and right brain hemispheres
- Smaller corpus callosum linking hemispheres
These areas are vital for emotions, reasoning, language, impulse control, and social skills.
Functional Changes
- Weakened neural pathways for emotional control, empathy, and distress tolerance
- Hyperactivity in fear response centers like the amygdala
- Imbalance between survival “lower brain” and “higher order” centers
- Difficulty toggling out of fight-or-flight mode
Together, these brain differences contribute to the challenging behaviors seen with reactive attachment disorder. The earlier intervention begins, the better the chance to spark more normal neural development.
New Research on the Neurobiology of Attachment
Exciting new research is illuminating how secure attachment relationships help shape infants’ rapidly developing brains on a biological level. Findings show:
- Parent-child interaction patterns change gene expression, activating and deactivating key parts of the genome. Nurturing caregiving activates genes that dampen stress responses.
- Sensitive, attuned parenting boosts oxytocin (the “love hormone”) and lowers cortisol (the “stress hormone”), with lifelong impacts on managing stress.
- Loving touch releases neurotransmitters that stimulate nerve growth and build pathways for emotions like trust and empathy.
- Attentive caregiver behaviors (eye contact, soothing voices, etc) help synchronize child brain wave patterns for calm, focused thinking.
- Responsive relationships build thick myelin coatings on nerve fibers for efficient neural conduction.
Together, this shows just how essential consistent nurturing is for wiring healthy socioemotional functioning—right down to our DNA!
Helping Your Partner Understand Reactive Attachment Disorder
When one parent is primary caretaker to a child with reactive attachment disorder, it can strain the parental relationship. The non-primary parent may struggle to connect with the child or feel left out.
With good communication, education, and teamwork, you can overcome this bump in the road. Useful tips include:
- Share resources to get your partner up to speed on RAD. Discuss strategies together.
- Seek family counseling focused on parenting techniques, not just the child.
- Outline each of your strengths. Balance roles based on skills, not gender.
- Schedule one-on-one time for your partner and child to bond through play.
- Debrief meltdowns or difficulties together after the fact, not in the moment.
- Have your partner manage self-care times for you like exercise class or a long bath.
- Say thank you. Show appreciation for each other’s hard work.
- Connect as a couple too. Prioritize date nights without kids.
You each bring something unique to the table. With empathy and balance, you’ve got this!
Should Siblings Attend Reactive Attachment Disorder Therapy?
If one child has reactive attachment disorder, including their siblings in treatment can have big benefits:
- Siblings gain education about RAD. This leads to greater empathy.
- Therapists can coach healthy interaction styles to use at home.
- Seeing their sibling get attention from participating provides motivation.
- Joint sessions allow safe space to address conflicts.
- Play therapy together lays groundwork for improved bonding.
- Siblings feel valued and included in the process.
But whole-family sessions aren’t always best. Consider your children’s specific needs. Often, a mix of individual and sibling joint sessions allows each child to benefit.
Discuss options with your therapist. With creativity, siblings can become a pivotal part of each other’s healing—not left out. Finding the right balance pays off.
Traveling Tips for Vacations with Reactive Attachment Disordered Children

Vacations require adjusting to new places and routines—challenging for kids with reactive attachment disorder. With thoughtful planning, you can reduce travel stresses and enjoy quality time together.
In Advance
- Have your child help pack their luggage. Pack familiar items.
- For plane trips, familiarize them with airport sights and sounds through videos.
- Book accommodations with kitchens when possible. Familiar food helps.
- Pack your child’s schedule, social stories, medications, and calming items.
En Route
- Build in generous extra time for transit, security lines, meal stops, etc.
- Bring engaging activities like small toys, books, electronics with headphones.
- Prevent hunger/thirst meltdowns by packing favorite snacks.
- Give frequent updates so your child knows what to expect next.
At Your Destination
- Ease the transition with familiar bedtime routines. Use a sound machine.
- Balance downtime with gentle exploration of new places. Take it slow.
- Process reactions afterward. “How did the beach make you feel?”
With the right planning, vacations can be relaxing and full of shared moments to look back on fondly. You’ve got this!
Tips for Managing Holidays with Reactive Attachment Disorder
For most families, holidays are treasured quality time. But their disruption from routine can be very difficult for kids with reactive attachment disorder. With some adaptations, you can minimize stress.
Prioritize consistency. Keep daily schedules, bedtime routines, and family traditions as similar as possible.
Prepare your child. Explain holiday expectations and events in advance with social stories. Practice opening gifts, greeting relatives, etc.
Involve your child. Have them decorate, cook holiday dishes together, or assign a special role. It promotes investment.
Allow choices. Let your child decide on an outfit, activity, or gift within structured options to give them autonomy.
Keep gatherings brief. Limit visits with relatives and friends. Take breaks to unwind together.
Offer quiet spaces. Have calming activities handy in case your child gets overwhelmed and needs an escape.
Expect setbacks. Holidays often lead to attachment regressions. Don’t lose hope! Just provide extra empathy.
With planning and flexibility, you’ll find ways to make the holidays meaningful while keeping stress low.
Reactive Attachment Disorder in the Classroom: Tips for Teachers

Reactive attachment disorder can make succeeding in a classroom environment difficult. But with preparation and awareness, teachers can make school feel safer for kids with RAD. Useful strategies include:
- Provide advanced notice of changes to class routines or schedules. Consistency is calming.
- Seat the student close to the front for more individual attention.
- Offer movement breaks. Supervised errands or stretching helps reset the nervous system.
- Allow calming objects like stuffed animals, fidget toys, headphones, and more as needed.
- Reward good behavior with immediate praise vs. stickers/tokens that seem arbitrary.
- Use simple, clear language and demonstrate tasks.
- Collaborate closely with parents and physicians. Track what works.
- If needed, develop a behavior intervention plan addressing triggers and responses.
- Get attachment disorder training through continuing education programs.
With the right support, school can help kids with reactive attachment disorder build social skills, independence, and self-esteem. Communication is key!
Finding Residential Treatment for Severe Reactive Attachment Disorder
If your child’s reactive attachment disorder is severe, residential treatment facilities provide specialized 24/7 clinical care. While difficult, this level of support is sometimes needed to help kids:
- Develop basic life skills
- Learn to self-regulate emotions and behavior
- Build healthy social functioning
- Process past trauma safely
- Prepare for successful home and school reintegration
Look for programs with:
- Attachment-focused psychotherapy and family therapy
- Attachment-based behavioral interventions
- Access to schools, recess, and group activities
- Credentialed staff experienced with RAD and trauma
- Warm, structured environments with sensory supports
- A track record of positive outcomes
Leaning on residential care temporarily does not make you a failure! It simply provides extra help so your child can thrive back home. Stay involved through family therapy.
Paying for Reactive Attachment Disorder Treatment

Effective reactive attachment disorder treatment often requires extended time in specialized therapy. That gets expensive fast. To access the care your child needs:
- Call your health insurer and explain the diagnosis. Push for coverage.
- Look into Medicaid, state insurance, and other public assistance if income eligible.
- Use Flexible Spending Accounts (FSA), Health Savings Accounts (HSA), or grants.
- See if therapists offer sliding scale fees or payment plans. Look for those who accept Medicaid.
- Consider borrowing against your 401k or future inheritance. This offsets out-of-pocket costs now.
- Set up an online fundraiser detailing your child’s needs. Friends and family want to help.
- Take advantage of free early intervention resources while waiting if needed.
Don’t lose hope! Where there’s a will, there’s usually a way. With creativity and advocacy, you can access the treatment your child deserves.
Activities to Build Trust with Reactive Attachment Disordered Children
For kids with reactive attachment disorder, rebuilding trust in caregivers requires showing up consistently, day after day. Special one-on-one playtime strengthens bonds. Try:
- Crafts or art projects – The physical closeness and joint attention builds rapport.
- Sensory activities – Playdough, kinetic sand, finger painting, etc. soothes.
- Outdoor exploration – Nature walks, playground time, or bike rides change the scenery while you chat.
- Reading together – Let your child choose themes that interest them.
- Listening to music or dancing – Being silly together brings laughter and connection.
- Board games – Turn-taking and joint participation teaches social skills.
- Cooking or baking – Guiding your child through measuring and stirring teaches cooperation.
- Practicing hygiene routines – Make bathtime fun with bubble baths, favorite toys and songs to relax.
- Imaginative play – Show you can meet them in their world. Imitate their made-up games.
Consistency and creativity builds trust! Let your child take the lead in showing you their interests.
Reactive Attachment Disorder in Adults

Without early treatment, reactive attachment disorder often persists into adulthood. Adults with RAD struggle with:
- Difficulty developing intimacy in relationships
- Social isolation
- Trouble reading social cues
- Anxiety, depression, and low self-esteem
- Anger issues
- Addiction or self-harm tendencies
- Chronic emptiness and sadness
But healing is possible! Intensive therapy focused on restructuring attachment patterns and processing developmental trauma can help adults with RAD improve relationship capacities. Key techniques include:
- Cognitive behavioral therapy (CBT)
- Dialectical behavior therapy (DBT)
- Eye movement desensitization and reprocessing (EMDR)
- Sensorimotor psychotherapy
- Joining support groups to practice social relating
With time and dedication, adults can overcome early attachment ruptures. It’s never too late to create meaningful bonds.
Reactive Attachment Disorder in Marriage
Partners with reactive attachment disorder often struggle to develop intimacy and trust in marriages and long-term relationships. Their trauma histories make opening up emotionally difficult.
For the non-RAD spouse, this can feel isolating and frustrating. But with work, empathy, and professional support, couples can overcome attachment issues together. Useful tips include:
For the RAD spouse:
- Share your attachment history with your partner. Explain what intimacy means to you.
- Challenge the impulse to shut down. Vulnerability gets easier with practice.
- Notice your partner’s efforts. Express genuine appreciation.
- Participate actively in marriage counseling.
For the non-RAD spouse:
- Learn about RAD’s relationship impacts. Don’t take detachment personally.
- Start small. Sharing little joys and sorrows builds trust over time.
- Reassure your partner often. Consistency helps counter avoidance.
- Respect their boundaries. Don’t force intimacy faster than comfortable.
- Care for your own needs too. Enlist support so you don’t burn out.
With work, empathy, and professional support, couples can overcome attachment issues together. Understanding RAD’s impacts allows you to rebuild your marriage stronger than ever.
























:max_bytes(150000):strip_icc()/social-anxiety-disorder-symptoms-and-diagnosis-4157219-5c5db04146e0fb000127c7e9.png)
:max_bytes(150000):strip_icc()/what-is-social-anxiety-disorder-5087486-Final-2cbb9bd5dd3b4b4a869a7dc5701ccd38.jpg)
.png?ixlib=gatsbyFP&auto=compress%2Cformat&fit=max&w=903&h=600)


:max_bytes(150000):strip_icc()/coping-with-social-anxiety-disorder-3024836_final-9e513fa6770b4548b5f61d5c0d2ea079.png)







:max_bytes(150000):strip_icc()/psychosis-vs-schizophrenia-5095195_final-42cb304e269948519136e8f0f4cdc0da.jpg)







:max_bytes(150000):strip_icc()/negative-symptoms-in-schizophrenia-2953123_FINAL-ef951f16569040e480dd672d00697f7f.png)



























:max_bytes(150000):strip_icc()/what-is-an-attachment-disorder-4580038_FINAL22-a5fcad506fa6456d88c35fa6d316afb7.jpg)





















