Understanding Schizophrenia
Symptoms, Causes, and Treatments
Schizophrenia is a serious mental illness that affects how you think, feel, and behave. It can seem scary, but with the right treatment and support, many people can manage their symptoms and live full, productive lives. This guide will help you understand the signs of schizophrenia, what causes it, and the various treatment options available.
What Is Schizophrenia?

Schizophrenia is a chronic brain disorder that affects about 1% of the population. It typically emerges in the late teens to early adulthood. The main symptoms of schizophrenia fall into three categories:
Positive Symptoms
These refer to experiences that most people do not normally have. They include:
- Hallucinations – seeing, hearing, smelling, or feeling things that are not really there. Hearing voices is the most common hallucination.
- Delusions – fixed, false beliefs not based in reality that the person firmly holds even when presented with contradictory evidence. Common delusions include paranoia or the belief that someone is plotting against them.
- Disordered thinking – disjointed and illogical thought patterns. The person may jump between topics unrelated to the conversation. Their speech may be jumbled and hard to follow.
- Movement disorders – repetitive, unintentional body movements such as rocking, twitching, or grimacing.
Negative Symptoms
These refer to abilities that are normally present but diminished or absent in schizophrenia. They include:
- Apathy and lack of motivation – loss of drive, energy, and interest to engage in goals or activities. The person may neglect self-care and hygiene.
- Social withdrawal – preference for solitary activities, reduced interaction with others. They may become isolated.
- Difficulty experiencing pleasure – reduced capacity to enjoy previously pleasurable activities. The world seems dull.
- Cognitive impairments – trouble with focus, certain types of memory and decision-making.
Disorganized Symptoms
These impact the person’s speech and behavior:
- Disorganized speech – incoherent manner of speaking where thoughts are loosely connected. Answers may be completely unrelated to questions.
- Disorganized or abnormal motor behavior – difficulty with goal-directed tasks, inappropriate childlike silliness, agitation, or unpredictable and uncontrolled movements.
The combination and severity of schizophrenia symptoms varies from person to person. Symptoms may build gradually over months or years, or there may be sudden onset of psychosis.
Schizophrenia Subtypes
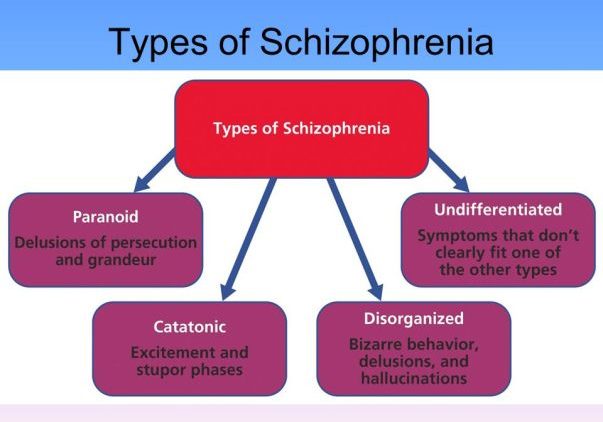
There are several subtypes of schizophrenia based on the predominant symptoms. These include:
- Paranoid schizophrenia – dominated by delusions and hallucinations. Paranoia is a key feature.
- Disorganized schizophrenia – primarily negative and disorganized speech and behavior. Emotions may be inappropriate.
- Catatonic schizophrenia – main features are disrupted motor behavior. This can include holding still in unusual postures for long periods, excessive and purposeless movement, or mimicking others’ speech and movements.
- Undifferentiated schizophrenia – mixed severe symptoms of multiple types.
- Residual schizophrenia – presence of past symptoms but currently milder intensity.
It’s possible for a person to transition between subtypes, and have overlapping symptoms. The subtypes help guide treatment plans.
What Causes Schizophrenia?

Researchers still don’t know the exact causes of schizophrenia, but it likely arises from a complex combination of factors:
Genetics
Schizophrenia has a strong hereditary component. Having a close family member with schizophrenia increases your risk. Specific genes may make someone more vulnerable.
Brain Chemistry and Structure
Imbalances in brain chemicals like dopamine and glutamate are thought to play a role. Differences in brain anatomy and neural connections have also been noted.
Prenatal and Perinatal Factors
Exposure to viruses or malnutrition in the womb, complications during birth, and other prenatal influences may increase susceptibility.
Psychological and Social Factors
High stress, childhood trauma and adversity, drug use, and social isolation are possible contributors, especially in triggering initial psychotic episodes.
Schizophrenia seems to arise from both genetic predisposition and environmental influences. Current thinking is that it’s a neurological disorder rooted in brain development and chemistry.
Schizophrenia Symptoms in Teens

Schizophrenia onset is typically between ages 16-30 for men, and 25-35 for women. But mild symptoms can emerge earlier in the teen years and include:
- Social withdrawal and isolation from peers
- A drop in academic performance
- Irritability or depressed mood
- Sleep disturbances
- Odd, vague, or irrational thoughts and beliefs
- Deterioration in self-care and hygiene
- Suspiciousness and extreme sensitivity to criticism
If your teen is displaying persistent behavioral changes, it’s important to have them evaluated by a mental health professional. Early intervention improves outcomes.
When to See a Doctor

Seek medical help if you notice any signs of psychosis in yourself or a loved one, such as:
- Hearing or seeing things others can’t
- False beliefs that seem strange or illogical
- Incoherent speech
- Extreme paranoia
- Dramatic changes in sleep, mood, or behavior
Sudden onset of psychosis symptoms warrants an urgent trip to an emergency room. For gradual onset of symptoms, make an appointment with a psychiatrist or mental health clinic. Early treatment is key to better management.
Schizophrenia Diagnosis
There is no single test for schizophrenia – a psychiatrist makes the diagnosis based on reported symptoms and observed behavior. They will evaluate for:
- Hallucinations, delusions, disorganized speech or behavior – These are the primary indicators of psychosis, and positive symptoms like hallucinations can only be assessed through a clinical interview.
- Time course – Symptoms must persist for at least 6 months and include 1 month of active psychosis. This helps rule out brief psychotic episodes caused by other factors.
- Ruled out other possible causes – The doctor will check for brain injuries, drug side effects, thyroid issues, mood disorders, and neurological conditions that could mimic schizophrenia.
- Significant dysfunction – Impairments in work, relationships, self-care and daily activities. Schizophrenia is highly disabling.
- Psychiatric history – Previous episodes, relationship to substance use, childhood issues, and treatment response.
Diagnosis guides treatment, so being open with your doctor is important. Keeping a record of symptoms can help with an accurate diagnosis.
Schizophrenia or Psychosis?
:max_bytes(150000):strip_icc()/psychosis-vs-schizophrenia-5095195_final-42cb304e269948519136e8f0f4cdc0da.jpg)
Psychosis is a broad symptom referring to a disconnected from reality. The hallmarks are delusions and hallucinations.
Schizophrenia is a specific mental disorder diagnosed when someone displays:
- Psychosis along with other characteristic symptoms
- Persistence of symptoms for over 6 months
- Significantly impaired functioning
So psychosis can occur in schizophrenia, but also in other conditions like bipolar disorder or drug use. Schizophrenia always involves psychosis, but not all psychosis is due to schizophrenia.
Schizophrenia Testing and Screening

In addition to a psychiatric evaluation, your doctor may recommend tests to identify any underlying factors that could contribute to symptoms, or rule out other possible causes. These can include:
- Medical history and exam – identifying any illnesses, medications, drug use, or brain injuries.
- Lab tests – such as for thyroid dysfunction, syphilis, and certain nutrient deficiencies.
- Psychological assessments – tests for IQ, memory and learning capacity, problem solving, social cognition.
- Brain scans – CT, MRI, or PET scans to detect any structural or functional brain abnormalities.
- EEG – to analyze electrical activity that could signal abnormalities.
While these tests don’t diagnose schizophrenia itself, they provide insight to guide appropriate treatment.
Early Signs and Symptoms

It’s common for schizophrenia symptoms to emerge gradually, starting with early warning signs that something is amiss. Being attuned to changes in thoughts, feelings, and behaviors can aid early intervention. Signs to look out for include:
In teens:
- Withdrawing from friends and activities
- A drop in academic performance
- Trouble thinking clearly or concentrating
- Suspiciousness and extreme sensitivity to criticism
- Deterioration in hygiene or personal care
- Odd or irrational beliefs
In young adults:
- Social isolation and lack of motivation
- Difficulty sleeping and decline in energy
- Difficulty experiencing pleasure
- Depressed mood
- Odd speech or ways of thinking
- Heightened uneasiness around others
Other early symptoms:
- Irritability or agitated behavior
- Lack of focus and trouble starting tasks
- Feeling tense and “on edge” frequently
- Not showing much emotion or inappropriate emotional responses
By tuning into early shifts in mood, thinking, and behavior, intervention can happen more quickly.
When to Seek Emergency Treatment

While schizophrenia develops gradually in many people, some experience a rapid onset of severe psychosis requiring emergency care. Symptoms signaling the need for urgent treatment include:
- Suicidal thoughts or plans – Psychosis elevates suicide risk. Thoughts of harming oneself warrant an ER visit.
- Intense paranoia or aggression – Delusions can spark volatile, unpredictable behavior that poses a safety risk.
- Inability to care for oneself – If hallucinations or delusions prevent independent functioning, hospitalization may be needed.
- Dangerous or bizarre behavior – Acting violently, displaying extremely disorganized/unsafe conduct also requires emergency intervention.
- Catatonia symptoms – Going into a stupor, rigid positioning, refusing to speak or eat needs immediate medical help.
Don’t hesitate to call 911 or seek hospitalization if schizophrenia symptoms become an imminent health or safety concern. With support, the situation can stabilize.
Prodromal Schizophrenia: Early Signs and Symptoms

In the months or years before a first psychotic break, many people experience subtle changes that mark early schizophrenia onset. This “prodromal” phase involves milder versions of schizophrenia signs. Recognizing them can enable early intervention which improves outcomes. Prodromal symptoms include:
Thinking and perception:
- Odd ideas or magical thinking
- Unusual perceptions like sensing random noises or shadows
- Poor concentration and distraction
Mood and behavior:
- Social isolation and withdrawal
- Irritability
- Depression
- Lack of motivation
- Drop in school or work performance
Speech and communication:
- Rambling speech
- Trouble communicating thoughts logically
Physical:
- Changes in sleep and energy
- Reduced hygiene or self-care
- Sensitivity to stimuli like light or sound
Tuning into subtle shifts in cognition, behavior, and functioning could spur seeking help before psychosis emerges. Early therapy can ease the transition to schizophrenia.
Positive Symptoms of Schizophrenia

The “positive symptoms” of schizophrenia refer to disturbances normally not present in healthy people. Hallucinations, delusions, thought disorders and movement issues reflect an excess or distortion of normal functions. Positive symptoms include:
Hallucinations:
- Hearing voices or sounds that aren’t real
- Seeing things that do not exist
- Smelling odors with no source
- Feeling sensations like touches with no cause
Delusions:
- Belief in things proven untrue
- Paranoia or belief in conspiracies against them
- Grandeur – over-inflated sense of self
- Thought broadcasting – believing their thoughts are audible to others
Thought disorders:
- Jumping between unrelated topics
- Tangential or nonsensical reasoning
- Word salad – mixing random words lacking meaning
Movement disorders:
- Agitated body movements and restlessness
- Muscle rigidity or loss of voluntary movements
- Tremors, ticks, grimacing, or stroking motions
Positive symptoms arise from an excess or distortion of normal functions and can be disabling. But many respond well to antipsychotic medications.
Common Schizophrenia Delusions

Delusions are firmly held false beliefs that remain fixed even when the person is presented with contradictory evidence. They are a core “positive symptom” of schizophrenia. Common delusional themes include:
- Persecutory delusions – belief that others are plotting harm or conspiring against them. This can spark mistrust and isolation.
- Delusions of grandeur – overblown sense of self-importance and power. The person may believe they have special talents or are on an important mission.
- Delusions of control – feeling thoughts or actions are being imposed by outside forces against their will. Common examples are believing thoughts are being inserted or broadcast.
- Somatic delusions – false beliefs about health and body functioning, like believing a body part is diseased or doesn’t belong to them.
- Delusions of reference – innocuous events or details seem connected to or have personal meaning for them. For example, believing news reports contain secret messages.
- Erotomanic delusions – a belief that someone famous or of higher status is in love with them.
Delusions often fuel paranoia and social isolation. But psychotherapy and antipsychotics can help ease them.
Hallucinations Symptoms and Types

Hallucinations involve seeing, hearing, smelling, tasting or feeling something that isn’t really there. They are common positive symptoms of schizophrenia that can feel intensely real and frightening. Hallucination types include:
- Auditory hallucinations – hearing voices or other sounds like music. Hearing voices is the most common schizophrenic hallucination.
- Visual hallucinations – seeing people, objects, or scenes that don’t exist. These are less common in schizophrenia.
- Olfactory hallucinations – smelling odors like smoke, rotten food, or chemicals.
- Gustatory hallucinations – tasting flavors without eating or drinking. These are rare.
- Tactile hallucinations – feeling touches, temperature changes, or things crawling on one’s skin with no physical cause.
Hallucinations feel real to the person experiencing them. But they aren’t voluntary. Learning to recognize them as symptoms can help. Most improve with antipsychotic medication.
Negative Symptoms of Schizophrenia
:max_bytes(150000):strip_icc()/negative-symptoms-in-schizophrenia-2953123_FINAL-ef951f16569040e480dd672d00697f7f.png)
While positive symptoms reflect an excess of normal functions, negative symptoms represent a loss or deficiency of typical abilities. They include:
- Lack of motivation and drive – Losing interest in work, school, relationships, hygiene or goals.
- Blunted affect – Reduced emotional expression or reactions. Conversations may feel stale.
- Anhedonia – Decreased ability to experience pleasure from activities once enjoyed. A feeling that nothing matters.
- Asociality – Preference for being alone rather than social interaction. Isolation increases.
- Alogia – Reduced speech output. Short empty replies.
- Avolition – Difficulty starting or persisting in goal-directed behavior due to lack of motivation.
Negative symptoms greatly impact daily functioning, but tend to be more treatment-resistant than positive symptoms. Supportive therapy helps manage them.
Cognitive Symptoms of Schizophrenia

In addition to psychotic and negative symptoms, many people with schizophrenia experience cognitive deficits that impair daily functioning. These include:
- Attention problems – Difficulty focusing and maintaining concentration. Easily distracted.
- Memory issues – Trouble recalling details and learning new information. Working memory needed to use info is often affected.
- Slowed processing speed – Taking longer to understand, process and respond to information. Following conversations can be hard.
- Impaired executive functioning – Struggles with planning, problem-solving, regulating emotions, self-monitoring and other complex mental tasks.
- Social cognition challenges – Misinterpreting social cues and poor insight into how one’s behavior is perceived. Difficulty communicating.
Cognitive remediation therapy and structured supports can enhance mental processing. But cognition is often still impaired even when other symptoms stabilize.
Depression and Schizophrenia

Depression commonly co-occurs with schizophrenia, especially the negative symptoms of low motivation, reduced pleasure and social withdrawal. Other depression signs like sadness, tearfulness, appetite changes, fatigue and poor sleep are also common in schizophrenia.
Contributors to depression include:
- Psychosocial stress of dealing with symptoms
- Social isolation and stigma
- Negative symptoms like anhedonia
- Side effects of medications
- Overlap in brain chemical imbalances
Since depression exacerbates disability, it’s important to address through counseling for coping strategies and possibly antidepressants. The combination of schizophrenia and depression is associated with elevated suicide risk.
Suicidal Thoughts and Schizophrenia
Schizophrenia carries a risk of suicide estimated at 5-6% over a patient’s lifetime. Contributing factors include:
- Depression – Hopelessness and sadness enhance suicide risk.
- Social isolation – Feeling cut off from others removes support systems.
- Internal voices – Auditory hallucinations may command self-harm.
- Poor problem-solving – Cognitive deficits impair ability to see options.
- Substance abuse – Alcohol and drugs increase impulsivity and depression.
Warning signs include talking about death, feeling trapped, extreme guilt, or saying goodbye to loved ones. If you notice these, call a suicide hotline or seek immediate help to stay safe.
Disorganized Schizophrenia Symptoms

Disorganized schizophrenia involves severe thought and speech disorganization along with flat affect and strange, childlike behaviors. Symptoms include:
- Disorganized speech – Rambling incoherently between unrelated topics. Answers may be completely unrelated to questions. Conversations are nonsensical.
- Disorganized behavior – Difficulty completing goal-directed tasks, restless agitation, silly childish mannerisms, unpredictable behavior.
- Flat or inappropriate affect – Lack of emotional expression
The exact causes of schizophrenia are still unknown. Current thinking is that it likely arises from a combination of genetic, biological, psychological and environmental factors.
Genetic factors
- Having a close family member with schizophrenia increases your risk.
- Certain genes may make someone more vulnerable.
- But genes alone do not determine who develops schizophrenia.
Brain chemistry
- Imbalances in neurotransmitters like dopamine and glutamate may play a role.
- Differences in brain anatomy and neural connections have also been noted.
Prenatal and perinatal factors
- Exposure to viruses, malnutrition or stress in the womb can increase risk.
- Complications during birth and delivery can affect development.
Psychological and social factors
- High stress, childhood trauma and adversity are possible contributors.
- Drug use and social isolation may trigger initial psychotic breaks.
Other factors
- Autoimmune diseases and inflammation may increase susceptibility in some people.
- Cannabis use during teen years can increase risk of early onset.
While the exact causes are still unclear, research does show that both biological and environmental influences contribute to development of schizophrenia.
Schizophrenia Risk Factors

Certain factors are known to increase a person’s risk of developing schizophrenia. The more risk factors present, the higher the chance of manifestation. Key risk factors include:
- Family history of schizophrenia – Having a close relative with the disorder significantly increases risk.
- Genetics – Certain genetic mutations and gene variations boost susceptibility.
- Prenatal infections – Exposure to viruses, bacteria and malnutrition in the womb can increase risk of schizophrenia later in life.
- Pregnancy and birth complications – Hypoxia, preeclampsia, low birth weight and other perinatal problems may contribute risk.
- Drug use – Teen cannabis use and certain drugs like amphetamines and cocaine can increase odds of schizophrenia.
- Childhood trauma – Emotional, physical or sexual abuse in early life may act as a risk factor.
- Social isolation and immigration – Lack of support networks appears to increase susceptibility. Migrants face extra social challenges.
While risk factors contribute to odds, they do not mean someone will definitely develop schizophrenia. Many people have these risks but never manifest symptoms.
Schizophrenia in Men vs Women

There are some gender differences in schizophrenia onset, severity and symptoms:
- Age of onset – Typically earlier for men at ages 18-25 vs. women at 25-35.
- Severity – Men tend to have more severe symptoms and higher rates of negative symptoms and substance abuse. Suicide risk is also higher in men.
- Symptoms – Women tend to have more hallucinations and paranoid delusions. Men have more systemized delusions and flat affect.
- Course – Women tend to have better premorbid functioning and more remissions from acute symptoms than male patients over the illness course.
- Cognition – The cognitive deficits associated with schizophrenia appear more pronounced in men.
- Brain differences – Male patients show greater loss of gray matter volume while women show more metabolic abnormalities.
These differences may be influenced by hormonal and genetic factors along with psychosocial variables. But many symptoms overlap significantly between genders.
Schizophrenia Statistics and Facts
Schizophrenia is a serious disorder affecting all aspects of life. Key statistics about this condition include:
- Schizophrenia affects about 1% of the global population.
- Typical age of onset is late adolescence to mid 30s.
- Men tend to develop schizophrenia earlier than women.
- People with schizophrenia die an average of 10-25 years earlier than the general population, often due to co-occurring physical conditions.
- 20 million people worldwide are estimated to have schizophrenia.
- 5-6% of people with schizophrenia die by suicide.
- About 50% of people with schizophrenia are not receiving appropriate care.
- With proper treatment, 60-65% of people with schizophrenia improve significantly or recover.
- Schizophrenia results in an estimated $155 billion in direct healthcare costs and lost productivity globally per year.
Raising awareness and expanding access to care are needed to improve outlooks and reduce disability. Effective treatments are available.
Schizophrenia Treatment

Treatment for schizophrenia involves medication, therapy, social supports and lifestyle changes. Options may include:
- Antipsychotic medications – These dopamine-blocking medications are the primary pharmacological treatment. They help reduce psychotic symptoms like hallucinations, delusions and paranoia.
- Psychosocial therapy – Cognitive behavioral therapy, social skills training, family therapy and supported employment programs help people manage symptoms and regain functioning.
- Coordinated specialty care – Programs providing team-based psychosocial treatments and support services improve outcomes.
- Self-care and lifestyle changes – Eating nutritious meals, exercising, getting good sleep, reducing stress and avoiding drugs and alcohol support overall health.
- Support groups – Peer support provides connection, reduces isolation and aids recovery. Group therapy also helps.
With comprehensive and sustained treatment, the long-term prognosis for schizophrenia can be good. Many people stabilize enough to lead independent, meaningful lives.
Antipsychotic Medications for Schizophrenia

Antipsychotic medications are the cornerstone of schizophrenia treatment. By blocking dopamine activity, these drugs can reduce psychotic symptoms like hallucinations, delusions and disordered thinking. Antipsychotics are categorized as:
First generation (typical) antipsychotics:
- Examples are chlorpromazine, haloperidol, fluphenazine, perphenazine.
- Effective for positive symptoms but have more neurological side effects like tremors or restlessness.
Second generation (atypical) antipsychotics:
- Examples are clozapine, risperidone, olanzapine, quetiapine, aripiprazole.
- Seen as more effective with fewer extrapyramidal side effects but can cause weight gain and metabolic changes.
Long-acting injectables:
- Injections of antipsychotics like haloperidol or aripiprazole last for 1-2 weeks.
- Help ensure adherence in people who struggle with taking daily pills.
Finding the most effective antipsychotic with minimal side effects takes some trial and error. Newer generation drugs are often best tolerated.
Psychotherapy for Schizophrenia

Along with medication, psychotherapy is an essential part of schizophrenia treatment. Talk therapy provides tools for managing symptoms, enhancing functioning, preventing relapse and improving wellbeing. Options include:
- Cognitive behavioral therapy (CBT) – Helps identify unhealthy thought and behavior patterns and develop healthier coping strategies. Can reduce hallucinations and delusions.
- Cognitive remediation – Improves cognitive functioning through drills and exercises targeting attention, memory and planning.
- Social skills training – Builds skills needed for social interactions like starting conversations or interpreting cues through role play. Reduces isolation.
- Family therapy – Provides education and support for family members to optimize home environment. Addresses communication and relationships.
- Illness management skills – Teaches strategies for medication adherence, identifying triggers, preventing relapse, problem-solving.
Therapy combined with medication provides comprehensive tools for managing schizophrenia successfully day-to-day.
Hospitalization for Schizophrenia

Hospitalization may be needed during acute psychotic episodes where symptoms become severe and disabling enough to pose health and safety risks. Reasons include:
- Suicide risk – delusions or hallucinations may incite harming oneself. Being monitored in a hospital setting keeps one safe.
- Self-harm behaviors – Psychosis can spark reckless, dangerous actions that require intervention.
- Unable to care for self – Severe symptoms like catatonia may prevent independent functioning, eating, drinking or sleeping.
- Aggressive or volatile behavior – Hospitalization protects the person and others when delusions or paranoia cause acting out.
- Medication stabilization – Switching or adjusting medications requires close observation to minimize risks and achieve optimal dosing.
- Medical oversight for rapid weight loss – Some medications lead to substantial weight loss initially that requires monitoring.
The goal is to stabilize acute symptoms rapidly so hospital stays can be as brief as possible before transitioning back home.
Schizophrenia Inpatient Treatment Programs
Inpatient programs involve staying at a psychiatric hospital or ward while intensive schizophrenia treatment is delivered. Goals of inpatient treatment include:
- Stabilizing acute symptoms like psychosis, depression or mania.
- Adjusting medications to determine optimal dosing and combinations with minimal side effects.
- Providing a calm, structured and supportive environment to help reorient the person.
- Offering different therapies and classes to build coping skills.
- Improving daily functioning through motivation and rehabilitation activities.
- Monitoring health and safety if self-care is compromised.
- Developing transition and discharge plans for continued improvement after hospitalization.
Inpatient programs aim to stabilize individuals in crisis and build skills and supports for pursuing recovery after discharge.
Outpatient Treatment Programs
Outpatient programs deliver schizophrenia treatment while the person continues living at home and attending school or work. Options include:
- Medication management from a psychiatrist
- Individual psychotherapy
- Group therapy and social skills training
- Family therapy and education
- Case management for service coordination
- Day treatment programs providing structured activities and skill building
- Peer support groups and mentoring programs
- Supported employment programs
Outpatient treatment allows practicing and implementing skills in real-world settings. Continuity of care after hospitalization is vital to maintain stability.
Cognitive Behavioral Therapy for Schizophrenia
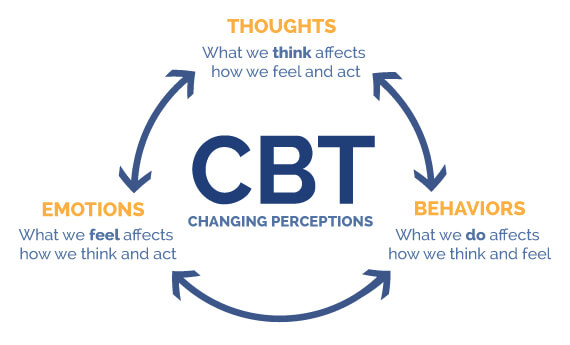
Cognitive behavioral therapy (CBT) is effective for reducing positive symptoms like hallucinations and delusions as well as associated anxiety and depression. It helps by:
- Identifying unhelpful thought and behavior patterns
- Recognizing symptoms as separate from self
- Evaluating the accuracy of distorted thoughts
- Considering alternative explanations
- Testing beliefs through reality checking experiments
- Promoting more constructive interpretations
- Reducing distress associated with symptoms
CBT provides problem-solving tools for managing hallucinations, voices, paranoia and other positive symptoms. It can improve functioning and quality of life.
Social Skills Training
Many people with schizophrenia experience social isolation and challenges interacting effectively with others. Social skills training aims to improve communication, relationship and coping abilities through techniques like:
- Practicing conversation skills – Initiating discussions, reciprocity, maintaining topics, nonverbal cues.
- Developing friendship skills – Learning to identify supportive peers, organize get-togethers, use humor appropriately.
- Mastering job-related skills – Interview practice, understanding workplace behavior norms, customer service etiquette.
- Interpreting social cues – Identifying relevant details like tone of voice or facial expressions and responding appropriately.
- Coping with criticism – Regulating emotions and having a constructive discussion when receiving negative feedback.
- Building problem-solving skills – Breaking tasks down into steps and considering multiple solutions.
Social skills training provides vital tools for forming relationships and navigating community and work environments successfully. Group classes allow practicing skills in a supportive atmosphere.
Vocational Rehabilitation

Schizophrenia often significantly impairs the ability to maintain employment. Vocational rehabilitation helps people regain job skills through services like:
- Supported employment – Specialized job training combined with ongoing coaching from a job counselor to facilitate success.
- Transitional work – Gradually increasing job duties and hours to build back skills at one’s own pace.
- Job social skills training – Instruction in workplace behavior norms, interviewing, interacting with supervisors and coworkers.
- Cognitive retraining – Exercises to improve memory, focus and executive functioning needed for work.
- Academic remediation – Assistance finishing high school or pursing higher education.
- Reasonable accommodations – Worksite adaptations matching capabilities like reduced hours, more breaks or a quiet office.
- Benefits counseling – Guidance on how income affects disability payments and healthcare to optimize employment.
Vocational rehabilitation provides the support and skill development needed to regain satisfying, enriching work adjusted to one’s abilities.
Schizophrenia Therapy and Counseling
Therapy and counseling equip individuals with tools and strategies for managing schizophrenia symptoms successfully. Benefits include:
- Learning to identify triggers and early warning signs to prevent psychotic relapses
- Building skills to cope with symptoms like hearing voices or paranoia
- Improving communication and social functioning
- Reducing distress associated with symptoms
- Developing motivation and goals that bring meaning and purpose
- Managing co-occurring issues like addiction or depression
- Getting support during periods of crisis
- Optimizing work and academic capacities
- Improving family relationships and dynamics
Therapy combined with medication and lifestyle changes enhances resilience. Ongoing counseling prevents setbacks.
Family Therapy and Schizophrenia
Family therapy helps relatives understand schizophrenia and identify how to best support their loved one. It focuses on:
- Psychoeducation – Information about symptoms, treatment, triggers, and early warning signs of relapse. Reduces stigma.
- Communication training – Improving supportive discussion while avoiding criticism and hostility. Setting clear expectations.
- Problem-solving – Collectively discussing challenges like treatment noncompliance and developing solutions.
- Coping strategies – Self-care tips for family members managing stress or disruptive behaviors. Establishing healthy boundaries.
- Recovery skills – Training family members to monitor medication, provide motivation, and reinforcement for functioning.
- Crisis prevention – Developing relapse prevention plans for getting help quickly during episodes of worsening symptoms.
Family therapy enhances the household environment, relationships and capacity to support ongoing improvement.
Schizophrenia Emergency Warning Signs
It’s important to know the warning signs indicating schizophrenia symptoms are worsening and require urgent assessment. Warning signs include:
- Hearing threatening or deteriorating voices
- Rapidly escalating paranoia
- Confused, disorganized thoughts and speech
- Significant changes in sleep or appetite
- Social withdrawal and isolation
- Depressed mood and expressions of hopelessness
- Increased agitation, hostility or volatile behavior
- Inability to care for oneself properly
- Talking about death, dying or suicide
If these signs emerge, contact a doctor right away to intervene early. Waiting risks symptoms becoming unmanageable. Getting help quickly optimizes outcomes.
Schizophrenia Relapse Prevention
Relapse prevention efforts aim to reduce the frequency and severity of symptom flare ups. Useful strategies include:
- Taking medications consistently, avoiding drug and alcohol use
- Monitoring mood and symptoms to catch warning signs early
- Having regular therapy and psychiatrist visits
- Reducing stress through relaxation exercises, socializing, good sleep habits
- Avoiding triggers that worsen symptoms like overstimulation
- Using coping strategies like distraction or talking to a support person
- Asking for help and using crisis services when symptoms spike
- Maintaining healthy habits like nutrition, activity and a daily routine
Preventing relapses enhances stability, functioning and quality of life. It takes commitment but yields major benefits long-term.
Outlook and Prognosis for Schizophrenia
With comprehensive treatment and supportive services tailored to the individual, the outlook for schizophrenia can be positive. Key factors influencing prognosis include:
- Early intervention – Shorter duration of untreated psychosis predicts better outcomes.
- Adherence with treatment – Those who stick closely to their medication and therapy regimen tend to have less residual symptoms and disability.
- Social and family support – Having an encouraging support network optimizes functioning and recovery.
- Absence of substance abuse – Eliminating drug and alcohol use improves prognosis.
- Age of onset – Developing schizophrenia in the teen or early adult years typically leads to better functioning than later onset.
- Response to treatment – Symptoms improving within 6 months indicates greater likelihood of remission.
While schizophrenia is chronic, many people achieve stability through comprehensive treatment and go on to lead productive, independent lives.
Schizophrenia in Children
It is rare for schizophrenia symptoms to emerge in childhood. More commonly, children may show developmental lags, learning disabilities or behavioral problems that sometimes precede onset of psychosis during the teen years or early adulthood. Signs in children may include:
- Social withdrawal and reduced interaction with peers
- Irritability, aggression or emotional outbursts
- Odd or regressive behaviors
- Decline in academic performance
- Speech or sensory abnormalities
- Difficulty concentrating
- Suspiciousness or paranoia
- Deterioration in hygiene
- Sleep disturbances
Children displaying a cluster of these behaviors should be assessed by a child psychologist and psychiatrist to determine appropriate interventions. Ongoing monitoring of social and cognitive development is also important.
Schizophrenia In Teens
Schizophrenia onset typically occurs during late adolescence and young adulthood. Warning signs in teens may include:
- Withdrawing from friends and activities
- Decline in academic performance
- Trouble thinking clearly or concentrating
- Odd ideas or magical thinking
- Increased sensitivity or irrational thoughts
- Deterioration in hygiene and self-care
- Sleep disturbances
- Depressed mood
- Extreme uneasiness around people
Early intervention improves prognosis. Seeking help at the first sign of symptoms can prevent worsening psychosis and impairment later on. Supporting healthy development is key.
Schizophrenia In Women

Schizophrenia affects women slightly differently than men. Unique aspects in women include:
- Later average onset – mid 20s to early 30s vs late teens to early 20s in men
- Better premorbid functioning – More likely to exhibit better social and academic adjustment prior to onset compared to males.
- More affective symptoms – Higher rates of psychotic depression and anxiety accompanying schizophrenia.
Support Groups for Schizophrenia
Support groups provide invaluable connection with others facing similar challenges. Benefits include:
- Reducing isolation and loneliness
- Sharing coping strategies for symptoms
- Offering illness management tips
- Providing empathy and hope
- Learning about community resources
- Making social connections for fun and friendship
- Reducing stigma through education and understanding
Both peer-lead mutual support groups and professionally-facilitated group therapy empower individuals and families. Support aids recovery.
Schizophrenia In Men

While schizophrenia affects both genders, men experience some unique differences including:
- Earlier average age of onset in late teens to early 20s.
- More severe symptomatology – higher rates of negative symptoms, depression, violence and substance abuse.
- Increased structural brain abnormalities and cognitive impairment.
- Earlier treatment initiation but reduced compliance with treatment long-term.
- More prominent social, occupational and self-care deficits.
Targeted supports and services addressing men’s needs can enhance engagement and prognosis.
Living With Schizophrenia
Though challenging, many people with schizophrenia live fulfilling, productive lives through comprehensive treatment and developing coping strategies such as:
- Taking medications consistently to control symptoms.
- Attending therapy and psychoeducation programs.
- Monitoring mood, sleep and symptoms closely.
- Reducing stress through relaxation skills, social connection and nature.
- Avoiding alcohol and recreational drugs.
- Engaging in work or school adjusted to meet abilities.
- Pursuing hobbies and activities that bring joy and purpose.
- Joining support groups to reduce isolation.
- Educating family and friends about schizophrenia.
- Asking for help during periods of worsening symptoms.
- Maintaining hope and optimism about one’s future.
With proper treatment and self-care, schizophrenia can be managed successfully.
Conclusion
Schizophrenia is a serious psychiatric condition, but not one without hope. Through medication, therapy, social supports and lifestyle changes tailored to the individual, many people achieve stability and live meaningful lives. Getting help early, avoiding substance use, and compliance with comprehensive treatment are key to the most favorable prognosis. Ongoing education, understanding and support enable those with schizophrenia to manage symptoms successfully and fulfill their potential.




